
Hemorrhoids are a disease in which there is blood stasis and abnormal changes in the veins of the rectum or in the area surrounding the anus. Such a delicate pathology has no restrictions with regard to the age category and gender.
The underlying factor leading to the formation of hemorrhoidal cones is stagnation, which, in turn, arises from a large number of other predisposing factors.
Pathology is characterized by characteristic symptoms that a person cannot ignore. The most specific clinical signs of hemorrhoids are itching and burning in the anal area, rectal hemorrhages, as well as severe pain in the perianal region.
The clinician will be able to establish the correct diagnosis based on a physical examination, but in addition, some laboratory and instrumental examinations may be needed.
Treatment of hemorrhoids directly depends on the severity of the course of the disease, which is why it can be both conservative and surgical.
Since pathology has quite a few varieties, it is coded with several meanings in the International Classification of Diseases.
Etiology
The main reason for the appearance of hemorrhoidal cones is:
- violation of the functioning of the vessels of this organ;
- increased arterial blood flow;
- disorder of the outflow of blood from the venous plexus;
- loss of tone of the veins of the rectum, which leads to their expansion and the appearance of nodes.
In addition, clinicians identify a huge number of unfavorable factors leading to the above processes, which is why they are usually divided into several groups - pathological and physiological.
The first category of causes of hemorrhoids includes:
- chronic constipation - hardened feces injure the walls of the rectum and anus;
- severe intoxication of the body - this should include poisoning with alcoholic beverages, toxic and chemical substances, as well as low-quality food;
- profuse diarrhea of an infectious nature;
- the formation of malignant, less often benign tumors in the intestine;
- diseases of the pelvic organs, such as prostatitis or cystitis;
- inflammatory diseases of the digestive system;
- hormonal disorders;
- portal hypertension and cirrhosis of the liver, as well as other ailments of this organ. The connection of hemorrhoids with the liver is due to the presence of common veins;
- the pathological influence of pathogenic bacteria that lead to the development of infections.
In addition to diseases and disorders, the causes of hemorrhoids may not be at all associated with the presence of one or another ailment in the body. Among the physiological factors, it is worth highlighting:
- lack of physical activity - this occurs against the background of a wide variety of sources - laziness, a severe illness that deprives the patient of the ability to move, as well as specific working conditions under which a person is forced to sit or stand most of the working time;
- excess body weight;
- poor nutrition - this includes the abuse of fatty, spicy foods, smoked meats, confectionery, carbonated drinks, semi-finished products, fast food and other harmful ingredients. It is for this reason that diet therapy is one of the components of the treatment of hemorrhoids;
- indiscriminate use of medications, including laxatives or oral contraceptives;
- incorrect performance of proctological diagnostic procedures or enemas;
- unconventional sexual preferences, namely anal sex;
- prolonged influence of stressful situations;
- performing heavy physical activity;
- engaging in some sports, in particular, cycling or motorbiking, equestrian sports and other types of weight lifting;
- excessive drinking and smoking of cigarettes;
- period of bearing a child or labor activity;
- menstruation.
Genetic predisposition plays an important role in the development of the disease. Diagnosing such a pathology in one of the closest relatives significantly increases the likelihood of bumps. Knowing this, you can independently prevent the appearance of an ailment, you just have to follow all the rules for the prevention of hemorrhoids.
Classification
By its clinical nature, the disease is:
- acute - this is the first manifestation of hemorrhoids that has not been previously diagnosed;
- chronic - characterized by alternating phases of exacerbation of symptoms and their retreat.
Depending on the area of formation of the hemorrhoid, cavernous pathology is divided into:
- external hemorrhoids - is such if a lump appears under the skin of the anus, and not under the mucous membrane of the rectum. It is considered the rarest form of the disease;
- internal hemorrhoids are the most common type of pathology in which the appearance of vascular cones directly in the anal canal is observed;
- mixed hemorrhoids - the second most common type of disease, which is characterized by the presence of signs of the two forms described above.
In addition, there are types of hemorrhoids, divided by severity:
- mild course - symptoms may be completely absent or be expressed to an insignificant degree. Conservative methods prevail in therapy;
- medium-heavy - differs in the addition of pain sensations, which are caused by an increase in nodes and their injury by feces. Internal bumps fall out during the act of defecation, after which they adjust themselves. It is possible to eliminate the disease with minimally invasive methods;
- severe - characterized by the expression of such a sign of hemorrhoids as bleeding. The nodes can fall out not only during bowel emptying, but also in any other situations leading to an increase in intra-abdominal pressure. In such cases, they can only be adjusted manually. The tactics of how to get rid of hemorrhoids can include both minimally invasive procedures and extensive operations;
- complicated - is expressed by an increase in the symptoms of the disease, and during the diagnosis, the development of complications is often observed, one of which may be thrombosis. However, it should be noted that not in all cases of untimely treatment of hemorrhoids, the formation of consequences occurs.
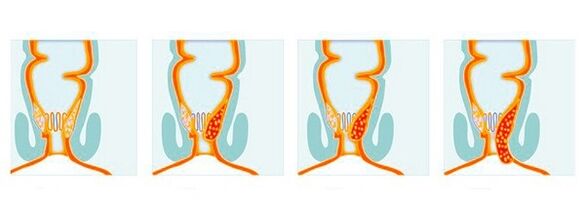
Symptoms
The first signs of hemorrhoids can be so minor that a person does not pay any attention to them. The initial clinical manifestations are considered to be:
- slight discomfort in the anus;
- non-intense itching of the anal area;
- pain during bowel movements;
- swelling of the entrance to the anal canal.
As the disease progresses, the following symptoms of hemorrhoids will begin to be expressed:
- burning and severe itching;
- increased pain, which will appear not only during bowel movements, but also during intense walking or prolonged sitting;
- the appearance of impurities of blood and mucus in the stool. It is noteworthy that pathological clots will not mix with feces, but are located on top of it;
- prolapse of the hemorrhoidal lump, which leads to severe pain;
- redness of the skin of the perianal region;
- rectal hemorrhages - if in the early stages such a sign of hemorrhoids could manifest itself only in the form of smearing with blood on toilet paper or underwear, then with a complicated course, the bleeding can reach the intensity of the stream. This is what often makes a person seek help.
In addition to specific clinical manifestations, the above symptoms of hemorrhoids can be supplemented by an increase in body temperature, which indicates the progression of the inflammatory process.
Diagnostics
It often happens that when symptoms of an ailment occur, a person does not know which doctor to contact for hemorrhoids. A proctologist or surgeon deals with the diagnosis and treatment of hemorrhoids, but for the first consultation, you can contact a therapist. It should be borne in mind that if the signs appear in a child, then it should immediately be shown to the pediatrician, and if in a pregnant woman, then first of all they consult an obstetrician-gynecologist.
The first stage of diagnosis includes the work of the clinician, which is aimed at:
- a detailed survey of the patient for the first time the signs of hemorrhoids appear - to identify the stage of the course of the disease;
- familiarization with the medical history and life history of not only the patient, but also his relatives - often this is enough to determine the sources of why hemorrhoids appear;
- conducting an objective examination aimed at assessing the state of the perianal region, as well as digital examination of the rectum, which will make it possible to distinguish internal hemorrhoids from external and determine the localization of the lump.
The second stage in establishing the correct diagnosis is laboratory examinations, namely, general, biochemical blood test and coagulogram.
The final part of the diagnosis is instrumental examinations of the patient, which are aimed at assessing how hemorrhoids look like, and provide for:
- sigmoidoscopy;
- anoscopy;
- colonoscopy;
- radiography using a contrast agent;
- Ultrasound of the abdominal organs.
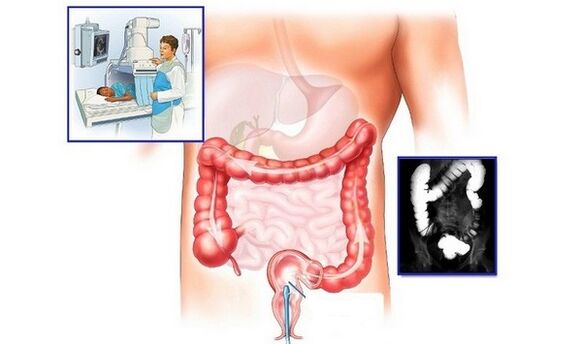
Only after studying the results of the examination, the clinician draws up tactics on how to cure hemorrhoids in a patient.
Treatment
The treatment regimen for the ailment will depend on the severity of the ailment, but common methods of treating hemorrhoids include:
- the use of medications for both local and general effects. In the first case, rectal suppositories, ointments, creams and gels are used, and in the second - tablets to improve blood circulation, strengthen veins and neutralize concomitant symptoms;
- adherence to a sparing diet - shown for both external and internal hemorrhoids. All recommendations regarding the menu and methods of cooking are provided by the attending physician;
- minimally invasive techniques for removing hemorrhoids;
- open surgery;
- the use of alternative medicine recipes. This includes the preparation of candles and ointments from natural ingredients at home, as well as decoctions from medicinal herbs and plants, which are used for ingestion or as microclysters and sitz baths.
Among the minimally invasive methods of treating hemorrhoids, it is worth highlighting:
- the introduction of sclerosing substances directly into the node;
- ligation with latex rings;
- infrared and electrocoagulation;
- cryodestruction;
- dearterization.
The tactics of removing hemorrhoids will be determined by the stage of the pathology.
With the ineffectiveness of conservative methods, as well as in cases of a complicated course of the disease, an open surgical operation is indicated - hemorrhoidectomy.
How to treat hemorrhoids in pregnant women and children will be prompted by an obstetrician-gynecologist and a pediatrician.
Possible complications
Ignoring pronounced clinical phenomena and late started treatment of hemorrhoids quite often leads to the development of the following consequences:
- accession of a secondary infection;
- the spread of the inflammatory process;
- insufficiency of the anal sphincter;
- profuse hemorrhages leading to anemia;
- proctitis and paraproctitis;
- the formation of blood clots;
- anal fissures.
Prevention and prognosis
To prevent the appearance of hemorrhoids, the following prevention rules must be observed:
- lead a healthy and moderately active lifestyle;
- eat right and balanced;
- strengthen the pelvic and abdominal muscles;
- take medications only as directed by your doctor;
- if possible, avoid physical and emotional stress;
- timely deal with constipation and other pathological causes of hemorrhoids;
- make sure that body weight is within normal limits;
- undergo a complete physical examination on a regular basis.
It is impossible to unequivocally answer the question about the prognosis of hemorrhoids, since the outcome depends on several factors - the stage and form of the course of the disease, the age category, the time of the start of hemorrhoid treatment and the patient's compliance with all the recommendations of clinicians.
Often people who have been diagnosed with hemorrhoids ask if it can go away on its own? The answer of doctors will always be negative - the disease will turn into a chronic form.
























